CALL US ON (03) 9897 4922 TO MAKE AN APPOINTMENT
KNEE
The knee is a complicated hinge joint. It is made up of bones, muscles, tendons and ligaments. These components in combination enable us to stand, sit, pivot and walk up and down stairs.
The most common disease to the knee joint is Arthritis. The word Arthritis literally means inflammation (‘Arth’ is joint, and ‘it is’ inflammation). There are several forms of Arthritis. Osteoarthritis is the most common form, and the knee is the most common joint affected.
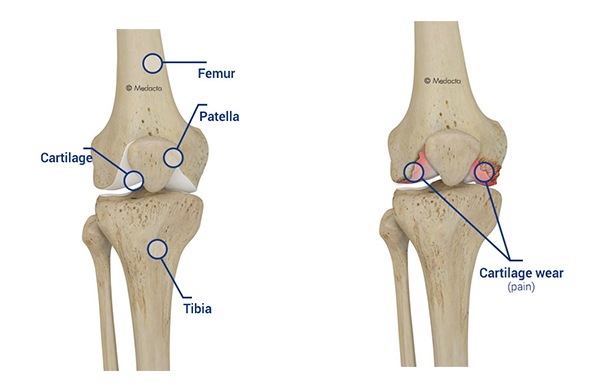
When the knee joint has been damaged by trauma or disease such as Arthritis, degeneration of the bony surfaces will occur.
The bony surfaces are covered with a protective skin called articulating cartilage. It is this protective coat that wears and causes raw bone to rub on raw bone.
Overtime the joint slowly erodes until the underlying bone is exposed. For the individual the knee becomes painful. This can manifest as swelling, instability, and discomfort.
Similar to hip surgery, knee surgery is indicated when you have advanced osteoarthritis of the knee joint and non-operative measures (eg. weight loss, anti-inflamatories , physiotherapy etc) are no longer controlling your pain.
TOTAL KNEE REPLACEMENTS
A Total Knee Replacement (TKR) procedure, also referred to as Total Knee Arthroplasty (TKA), is a surgical procedure which involves resurfacing your knee joint and replacing the arthritic parts with artificial metal or plastic prosthesis components.
The surfaces of the thigh and shin bones are replaced with high resistant metallic components called the femoral component and tibial baseplate. Between the femoral component and tibial baseplate a plastic insert is implanted.
This replaces the cartilage function allowing the thigh and shin bone to slide on each other. It is not to remove the whole joint, but merely to resurface the diseased or traumatised bony edges.

People with a stiff, painful knee that makes it difficult to perform even the simplest of movements and interferes with daily activities despite trying other non-operative measures such as anti-inflammatory medication, activity modification and joint rehabilitation exercises without significant improvement may be candidates for Total Knee Replacement Surgery.
POTENTIAL BENEFITS OF Total Knee Replacement SURGERY


The main benefits of a successful Total Knee Replacement are a significant reduction in the symptoms of arthritis.
These include:
A reduction in knee pain. The pain will be rapidly and dramatically reduced and usually eliminated.
Recovery of mobility. Your knee will function with less effort, almost regaining your original mobility.
Improvement in quality of life. Your everyday activities and your social life will no longer be limited by pain and reduced mobility.
Patient Specific Instrumentation (PSI)
Technical advances have given us new materials and new instrumentation to replace your problem knee. Mr Booth prefers to perform the knee replacement using patient specific instrumentation for most patients unless there is a specific reason otherwise. This involves analysing a diagnostic image of your leg and creating a surgical instrument in collaboration with a team of engineers that is tailored specifically to fit the exact shape of your knee.
Patient Matched Technology enables precise preparation of your bone in surgery for accurate implanting of the prosthesis leading to a less traumatic procedure and to ensure the knee replacement is well aligned.
Once Mr Booth has diagnosed that a Total Knee Replacement procedure is needed you will be required to have a CT scan of your leg at least 3 weeks prior to your scheduled surgery date.
A plastic 3D model is then created using the image of the CT scan. This enables Mr Booth to select the best implant for you. Using the 3D model of your knee Mr Booth then, in collaboration with a team of bio-medical engineers develops the surgical instruments to be used on your knee.
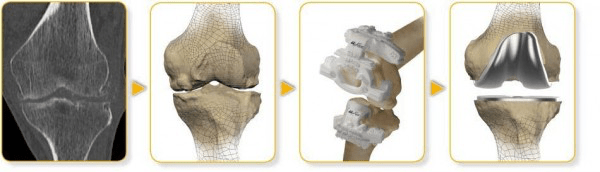
Mr Booth will receive these patient matched instruments along with a plastic replica of your knee prior to your surgery date.
Uni-compartmental Knee Replacements
Patients with osteoarthritis that is limited to just one part of the knee may be candidates for a uni-compartmental knee replacement (also called a “partial” knee replacement).
Your knee is divided into three major compartments: the medial compartment (ie. the inside part of the knee), the lateral compartment (ie. the outside part), and the patellofemoral compartment (ie. the front of the knee between the kneecap and thighbone).
In a uni-compartmental knee replacement, only the damaged compartment is replaced with metal and plastic. The healthy cartilage and bone in the remainder of the knee is left alone. The knee joint becomes worn-out most commonly as a result of osteoarthritis but may also result from other causes such as trauma or injuries, meniscal tears and overuse.
The aim of a UKR is to relieve pain, restore function and movement, and improve quality of life.
Potential benefits of a UKR
- Smaller incision
- Less bone removal
- Less blood loss
- Faster recovery
- Better range of movement
- More “natural” feeling knee
Disadvantages of a UKR
- Slightly less predictable pain relief
- Potential need for more surgery
For example, a TKR may be necessary in the future if arthritis develops in the parts of the knee that have not been replaced.
Not all patients are suitable candidates for a UKR. This will all be discussed with Mr Booth during your consultation.
KNEE ARTHROSCOPY
The word arthroscopy comes from two Greek words; Arthro (joint) and Scope (to look).
Knee Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. Using this technique, Mr Booth can visualise, diagnose and treat problems inside the joint.
An Arthroscopy is usually done through two small incisions around the knee, through which a camera and small instruments can be inserted into the knee to feel, repair or remove damaged tissue.
It is a minimally invasive procedure with most patients being admitted as outpatients, either in a hospital or in a day surgery centre. They have the procedure early in the day, and leave in the afternoon or early evening.
Mr Booth will usually perform an Arthroscopy when conservative treatment options e.g. physiotherapy, anti-inflammatory medications & corticosteroid treatment have not provided adequate improvement in pain levels.
Arthroscopic knee surgery may:
- Relieve pain
- Improve joint stability
- Delay the onset of osteoarthritis
- Delay the need for total knee replacement
- Improve your quality of life
- Make it easier to carry out your normal everyday activities
An Arthroscopy may be useful in evaluating and treating the following conditions:
- Meniscal Tears
- Loose Bodies
- Osteoarthritis
- Chondromalacia of the Patella
- Inflammatory Synovitis
- Cruciate Ligament Injury Assesments
- Local Cartilage Damage
ACL RECONSTRUCTION
An ACL injury is a tear or sprain of the anterior cruciate ligament. The ACL is one of the major ligaments in your knee.
ACL injuries most commonly occur during sports that involve sudden stops or changes in direction, jumping and landing — such as soccer, basketball, football and downhill skiing.
Injuring your Anterior Cruciate Ligament (ACL) is often acutely painful. Patients report that their knee ‘gives way.’
If ACL injury occurs during a game of sport, patients are usually unable to continue playing the game, although occasionally this is not the case and the injury can be subtle.
An audible pop may be heard, and the knee usually swells soon after the incident.
After the initial injury patients usually limp or struggle to put weight on the knee, but these early symptoms often resolve in 10-14 days.
Sometimes, the full extent of the injury can go unnoticed and often when the patients attempt to return to their previous sporting activity, they again experience giving way and a lack of confidence in the knee.

Treatment Options:
There are a range of treatment options for ACL rupture depending on your injury, personal history and goals.
Mr Booth will be able to discuss these in more detail at your appointment.
The ACL does not heal on its own, as such the ligament will need to be reconstructed.
To achieve this, a small ‘graft’ is obtained from another tendon in your leg and then inserted in place of the old, torn ACL.
Numerous graft options exist, including hamstrings, patella tendon and quadriceps tendon.
Each case is unique, and Mr Booth will discuss his recommendation for graft type for your injury in your consultation.


