CALL US ON (03) 9897 4922 TO MAKE AN APPOINTMENT
Hip
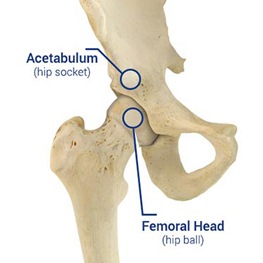
The hip joint is formed by the articulation of the rounded head of the femur and the cup-like acetabulum of the pelvis. It forms the primary connection between the bones of the lower limb and the axial skeleton of the trunk and pelvis.
The surface of the femoral head and the acetabulum, where the bones come in contact, is coated by a smooth tissue called articular cartilage. The cartilage, together with a substance called synovial fluid, prevents the bones from rubbing against each other and from becoming damaged.
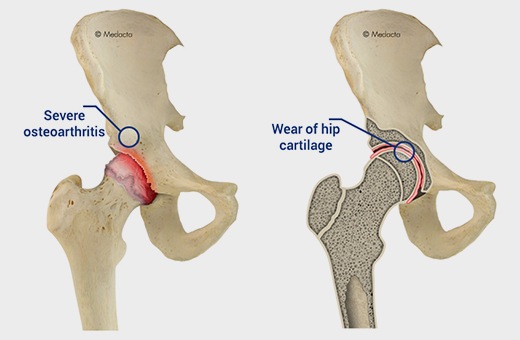
Arthritis of the hip
(the most common form of Hip disease)
The main cause of hip joint diseases is the wear of the articular cartilage: osteoarthritis. This wear causes pain, initially only when a load is bearing on the joint but over time it becomes painful more and more frequently eventually leading to constant pain even when resting.
The increase in intensity of the pain is a slow process, sometimes over many years, and can lead to a stiff hip joint.
WHO IS AFFECTED
Hip arthritis typically affects patients over 50 years of age. It is more common in people who are overweight, and weight loss tends to reduce the symptoms associated with hip arthritis.
There is also a genetic predisposition of this condition, meaning hip arthritis tends to run in families. Other factors that can contribute to developing hip arthritis include traumatic injuries to the hip and fractures to the bone around the joint.
Symptoms of Hip Joint Disease:
- Pain in the hip joint (usually felt in the groin area)
- Referred pain to the thigh and knee
- Limping
- Reduced range of motion
- Muscle stiffness
- Pain when trying to put weight through the leg on the affected side.
Causes of Hip Joint Disease:
It is clearly understandable when looking at the schematics how impingement occurs, the unknown question is why?
It is believed that many normal people have ‘bumps’ or slightly over-deep sockets and could potentially develop FAI – this is just the way we are built and develop.
But the hip has to also be provoked in some way to cause damage – this explains the tendency for athletes, sporting professionals and active people to be more susceptible to this form of injury.
Management of Hip Joint Disease:
An initial trial of non-operative treatment is advocated for most patients as the pain is relatively self-limiting. Lifestyle modification is the single most important factor including losing weight for many people.
For most this may result in resolution of symptoms but this will restrict attempts to return to sport. Use of painkillers and anti-inflammatories may temporarily help the pain.
Physiotherapy may reduce the local inflammatory reaction, improve core stability, improve soft tissue flexibility and assist in measures to avoid provocation but will not address the underlying mechanical problem.


Hip replacement surgery is a common treatment for severe osteoarthritis.
Successful hip replacement MAY bring dramatic pain relief and improvement in the function of the hip joint.
TOTAL HIP REPLACEMENT SURGERY
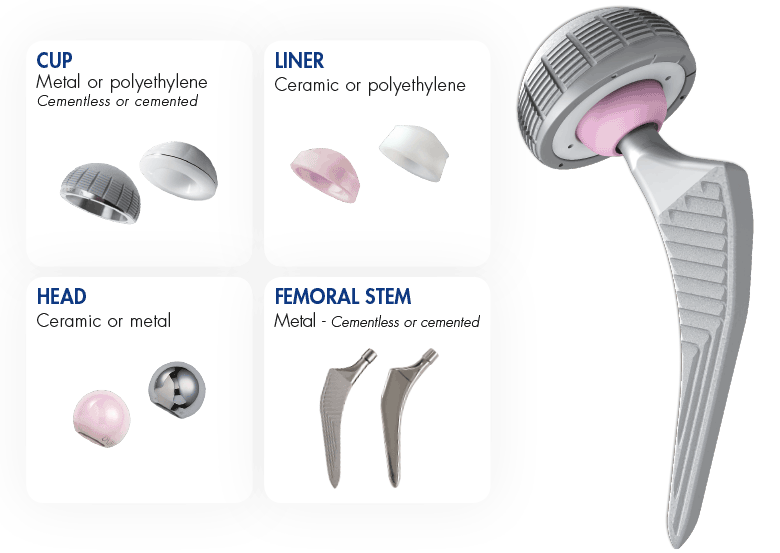
Total hip replacement surgery removes damaged or diseased parts of a hip joint and replaces them with new, man-made parts.
The goal of this surgery is to relieve pain, help the hip joint work better and improve walking and other movements.
Total hip replacement is a safe, reliable procedure that can relieve your pain and stiffness and return you to most of the activities that you enjoy.
There are several ways for a surgeon to perform total hip replacement surgery including (but not limited to):
- Posterior (Moore)
- Lateral (Hardinge or Liverpool)
- Antero-lateral (Watson-Jones)
- Minimally invasive
- The Anterior Minimally Invasive (Hueter) Approach
Some approaches are more muscle sparing than others leading to a quicker recovery however the most important aspect of any hip surgery is to ensure that the prosthesis is implanted accurately and correctly, that the surgery is carried out in an efficient manner minimising blood loss and reducing anaesthetic time and the risk of complications is kept to a minimum.
Remember that ALL approaches if performed correctly will result in a successful pain free outcome that should last at least 20-30 years using modern day implants.
The main benefits of a successful Total Hip Replacement are:
- Reduction in hip pain. The pain should be rapidly and dramatically reduced and usually eliminated.
- Recovery of mobility. Your hip will function with less effort, almost regaining your original mobility.
- Improvement in quality of life. Your everyday activities and your social life will no longer be limited by pain and reduced mobility
People with hip joint damage that causes pain and interferes with daily activities despite trying other treatments such as exercise, walking aids and medication without significant improvement may be candidates for hip replacement surgery.
This will all be discussed with Mr Booth at your consultation.


DIRECT ANTERIOR TOTAL HIP REPLACEMENT SURGERY
The direct anterior minimally invasive surgery approach in total hip replacement procedures is a surgical technique which follows an inter-muscular and inter-nervous plane to reduce the risk of injury to muscles, tendons, vessels and nerves.
By avoiding the nerves and because no muscles are cut, this can aid in rapid recovery for patients following surgery.
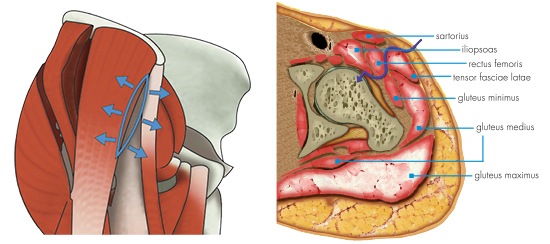
Mr Booth has extensive training in the direct anterior approach technique and routinely performs this approach for all total hip replacement procedures because it reduces the risk of injury to your muscles, tendons, vessles and nerves.
This means your recovery following surgery should be much more rapid compared to the other surgical approaches that involve cutting the muscle.
The procedure is performed in hospital. Your hospital stay is usually overnight but may be longer, depending on your individual circumstances.
The operation will take approximately 1.5 hours. The incision is approximately 7-10cm long. The incision is made over the top of your hip joint in the region of your groin.
The worn surfaces of the hip are removed and the surfaces are replaced with artificial components. Metal is used for all components however the bearing surfaces may vary depending on the circumstances: metal, ceramic, or plastic.
Ligaments and tendons are preserved so it is possible following a primary joint replacement to walk a few hours after surgery, fully weight-bearing on your new hip. In fact, it is something that we want you to do unless otherwise advised.


Potential Advantages of anterior total hip replacement surgery


- Reduced risk of dislocation
- The ability to sit in a normal chair immediately after surgery
- The ability to safely travel home by car at the time of discharge
- The ability to walk with minimal assistance in the days after surgery.
For older patients, particularly those that live alone, this facilitates a rapid return to independent living.
For younger patients, including manual workers this may enable a more rapid return to employment.


